Total Knee Replacement
Advanced knee replacement procedures
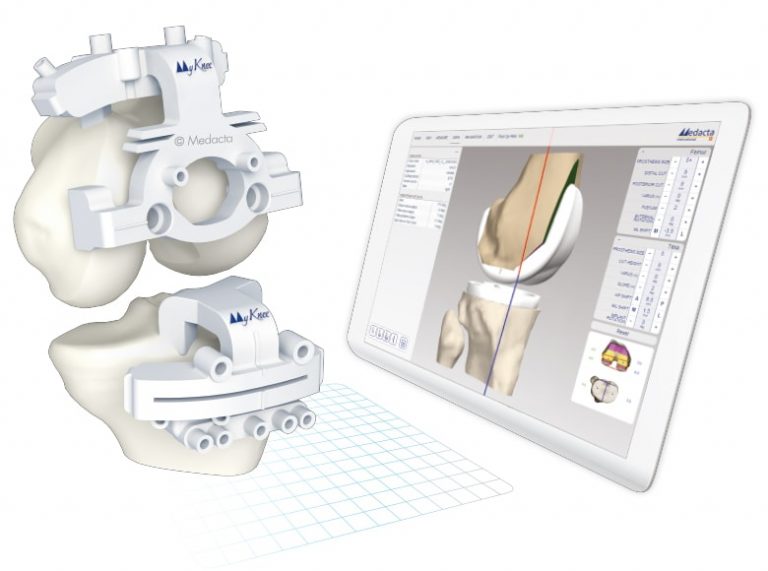
3D printed technology
Knee replacement, or knee arthroplasty, is typically recommended for individuals suffering from degenerative joint diseases such as osteoarthritis, rheumatoid arthritis, or post-traumatic arthritis, which cause severe pain, stiffness, and loss of mobility. These conditions result from the deterioration of cartilage that cushions the bones of the knee, leading to painful bone-on-bone contact.
Our approach incorporates 3D-printed patient-specific instruments (PSI), 3D anatomical mapping, augmented reality, and the kinematic alignment (KA) surgical technique. These technologies allow us to tailor each surgery to the individual’s unique anatomy, ensuring optimal implant alignment and the restoration of natural knee motion. By using 3D imaging to accurately map the knee joint, we create customised instruments that enhance the precision and effectiveness of the procedure.
Mr Freedman employs computer-assisted and augmented reality technologies during surgery to provide real-time feedback, which help to achieve optimal placement of the knee implants according to kinematic alignment principles. This personalised approach aligns the knee naturally and improves joint biomechanics, reducing postoperative discomfort and accelerating recovery.
The benefits of a total knee replacement
- Tailored Fit for Optimal Function: Our 3D-printed patient-specific instruments and detailed anatomical mapping help achieve precise alignment with your unique anatomy, promoting better joint function and longevity.
- Advanced Kinematic Alignment: Our kinematic alignment technique aligns the artificial joint to mimic your knee’s natural motion, reducing wear and enhancing comfort, allowing a more active lifestyle post-surgery.
- Real-Time Precision: Using augmented reality technology during surgery for real-time feedback on implant positioning. This cutting-edge approach increases the accuracy of the procedure, minimises risks, and improves surgical outcomes.
- Reduced Recovery Time: The precision and efficiency of our surgical techniques not only enhance the surgical outcome but also speed up the recovery process, allowing you to return to daily activities sooner.
- Durable and Effective: The advanced materials used in our implants help achieve excellent durability and function.

Case Examples
Mr Freedman’s training & experience

An Internationally-trained and renowned Orthopaedic surgeon, Mr Freeman brings over a decade of experience to providing a meticulous standard of care.
The success of technically complicated surgery depends on several elements, but one important factor is having a highly-trained and experienced surgeon.
Mr Freedman completed a fellowship in the UK to train in hip arthroscopy with Professor Damian Griffin, a world-renowned expert in hip arthroscopy and hip preservation surgery.
While on fellowship in the UK, Mr Freedman’s supervisor, Professor Griffin, received an invitation to observe a new hip replacement technique in Paris with Dr. Frederic Laude, a world expert in Direct Anterior hip surgery. As fate would have it, other commitments prevented Prof. Griffin from attending, so he sent Mr Freedman in his place, and he was amazed by the innovative procedure, the minimal incision, and the quick recovery of patients. Mr Freedman later returned to Paris to complete a fellowship under Dr Frederic Laude.
Upon returning to Australia, Mr Freedman, successfully implemented anterior approach hip replacements in his practice, leading to rapid growth in his case numbers and the eventual standardisation of this technique, even for complex surgeries.
-
Internationally Trained and Recognised
Mr Freedman has trained under some of the best hip surgeons in Europe.
-
Cutting-Edge Techniques
Mr Freedman employs advanced technology and techniques to ensure the best possible outcomes for his patients.

Advanced techniques, fantastic results
Frequently asked questions
The purpose of Total Knee Arthroplasty is to significantly reduce the symptoms of arthritis. These include:
- A rapid and significant reduction of knee pain.
- Recovery of mobility – your knee will move more smoothly again and will function more normally.
- Improvement in quality of life – Everyday activities such as walking and bending your knee will no longer be limited by pain and restricted mobility.
The terminology here is unfortunately confusing for patients!
In knee replacement/resurfacing any remaining worn cartilage and a few mm of bone are removed from the end of the femur (thigh bone) and the top end of the tibia (lower leg) bone. The muscles of the knee and collateral ligaments (side ligaments of the knee) are completely preserved. The worn cartilage is then replaced with a smooth prosthetic surface. The procedure is called a total replacement because all of the cartilage surface of the knee is covered with a new surface. In comparison, in a partial knee replacement only the cartilage on half half (ie. either inside or outside half) of the knee is resurfaced.
Our locations
- Main Practice Consulting Rooms
- Other Clinic Consultations
- Surgery Operating locations
- Telehealth Consultations
Our main practice consulting rooms are located at:
Mr Ilan Freedman
Suite 2, Monash House Private Hospital
271 Clayton Road, Clayton VIC 3168.
Driving: Monash House Private Hospital is situated on Clayton Rd, across the road from Monash Medical Clinic. Clayton Road is easily accessible form Princes Highway (Dandenong Rd, North Rd or Centre Rd).
Parking: Parking available onsite (paid – inexpensive) and neighbouring streets (free)
Public transport: 3 minutes walk from Clayton Railway Station. Bus stop directly outside.
Location in the hospital: We are located on the ground floor, opposite the hospital coffee shop and next door to Capital Radiology
Mr Freedman also consults regularly at the following clinics.
Mulgrave Private Hospital Consulting Suites
Address: Blanton Dr, Mulgrave VIC 3170
Parking: Inexpensive onsite parking
The Bays Private Hospital Consulting Suites – Mornington
Address: Vale St, Mornington, 3931
Parking: Free Parking Available on site
Location: We are located in Suite 15 at The Bays.
Warragul
Address: 33 Victoria Street, Warragul 3820
Parking: Free Street Parking
Maryvale Private Hospital
Address: 286 Maryvale Rd, Morwell, 3840
Parking: Free Street Parking
Bay Street Specialist Centre
Address: Suite 4, 214 Bay Street, Brighton VIC 3186
Parking: Free Street Parking
Mr Freedman’s surgery operating locations are:
Mulgrave Private Hospital
Address: Cnr Police Rd & Gladstone Rd, Mulgrave, 3170
The Bays Private Hospital, Mornington
Address: 262 Main St, Mornington VIC 3931
Monash House Private Hospital
Address: 271 Clayton Rd, Clayton VIC 3168
Maryvale Private Hospital
Address: 286 Maryvale Rd, Morwell VIC 3840
Telehealth Consultation
We are pleased to offer telehealth appointments, allowing you to consult with Mr Freedman from the comfort of your home. Whether for a follow-up, pre-surgical consultation, or orthopaedic advice, our telehealth services provide expert care without the need to travel. Using secure and easy-to-use technology, our telehealth appointments fit seamlessly into your schedule, ensuring the same high standard of care as an in-person visit.

Get back to life sooner
We understand that seeking care for your hip or knee condition is an important decision, and we are here to provide you with the support and expertise you need.
Please take a moment to fill out the following information so that we can better understand your needs and how we can assist you.
