Before Surgery
What to expect in your first meeting with Mr Freedman
We understand that the prospect of meeting with a surgeon and discussing potential surgery can be daunting. Our goal is to build your confidence and assure you that you are in the capable hands of a compassionate and highly skilled surgeon.
During your first visit, Mr Freedman will focus on diagnosing the source of your orthopaedic issue, educating you about the nature of your condition, and discussing management options to address your specific needs. Don’t be surprised if Mr Freedman gives you his full attention and doesn’t scribble a lot of notes during your consultation.
The diagnostic process during your initial consultation involves several key steps.
- Mr Freedman will begin by taking a detailed clinical history, asking about any relevant injuries, the onset and severity of symptoms, and factors that may aggravate or alleviate your pain.
- This discussion is accompanied by a physical examination, for which we recommend wearing loose clothing such as shorts or tracksuit bottoms.
- Initial investigations may also include X-rays to provide a baseline assessment of your joint, with further advanced imaging like CT or MRI scans ordered as necessary.
Mr Freedman uses an advanced clinical AI platform captures all of the clinical detail and your GP will usually receive a clinical summary before you arrive home from your consult.


Management strategies will be clearly outlined by Mr Freedman based on your clinical diagnosis.
- Whether surgical intervention is needed, further conservative treatment is advised, or additional investigations are required, you will leave with a comprehensive plan tailored to your needs.
- We invite family members or carers to accompany you during your visit to provide support and help in understanding the proposed treatments.
- As part of our commitment to advancing orthopaedic care, you may be invited to participate in research studies, though this is entirely voluntary.
Our priority is to ensure you feel informed, cared for, and confident about the next steps in your treatment journey. Contact us today to book your initial consultation.
What to Bring to Your First Appointment with Mr Freedman
The diagnostic process during your initial consultation involves several key steps.
- Doctor’s referral letter from your GP or medical specialist involved in your care.
- Any relevant radiology (X-ray, MRI, bone scan, etc) reports in your possession.
- An up-to-date list of your current medications.
- Any previous letters or documentation related to your condition.
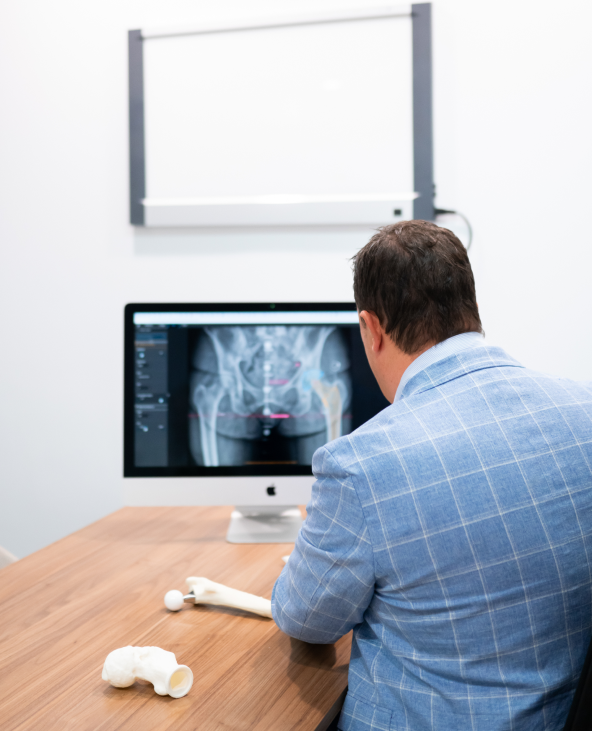
Thorough preoperative preparation will help optimise recovery from surgery. Completing all necessary evaluations and tests beforehand helps identify and address potential risks, minimising complications. Highlight any specific conditions you have, especially if you:
- Have a bleeding disorder.
- Have experienced blood clots in your legs (deep vein thrombosis) or lungs (pulmonary embolism).
- Are currently on any blood thinners.
- Have any heart or lung issues.
- Have diabetes (type 1 or 2).
- Have had a previous joint infection.
Additionally, if you are a smoker, it’s crucial to cease smoking prior to your surgery. Smoking can significantly increase the risk of surgical complications, including infection and delayed wound healing. Staying active is also beneficial; we encourage continuing low-impact exercise up to the time of your surgery to promote better recovery outcomes.
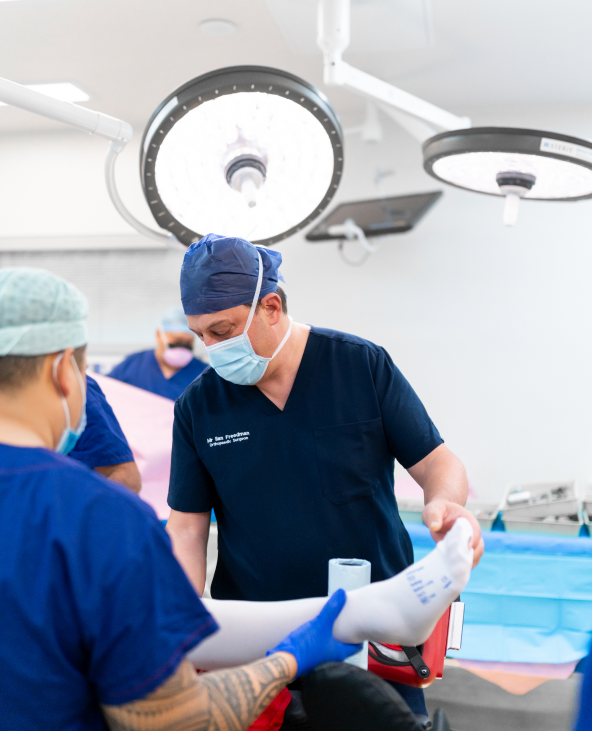
Mr Freedman's Enhanced Recovery Program
Optimal perioperative nutrition is crucial for enhancing the body’s healing capacity following surgery. Mr Freedman collaborates with leading scientists and nutritionists to ensure that his patients have access to the latest science, education and products to enhance muscle, wound and soft tissue recovery.
We will also give you access to technologies such as wearable cold-compress garments to reduce inflammation and reduce your requirement for pain medications.

Nutrition Before Surgery
Mr Freedman will provide further personalised advice during your consultation to help you optimise your nutrition and ensure a smooth recovery.
In the weeks leading up to surgery, optimising your nutrition is crucial for a successful recovery. Focus on:
- A balanced diet rich in high-quality proteins, complex carbohydrates, and healthy fats to support healing and energy levels.
- Ensure adequate intake of vitamins and minerals, particularly Vitamin C, Vitamin D, and Zinc, to boost immune function.
- Taking a nutritional supplement such as Mend Repair and Recover targeted blend of nutrients helps protect muscles and accelerates healing.
- Stay hydrated by drinking plenty of water and include fibre-rich foods for digestive health. Incorporate probiotics to maintain gut health and reduce inflammatory foods like processed snacks.
- Additionally, Dex, a medically formulated rapidly absorbed carbohydrate drink, can help keep your body nourished, hydrated, and in a state of building rather than breaking down protein.

Preparing Your Home
Preparing your home for recovery after hip or knee surgery is a crucial step to ensure a smooth and comfortable rehabilitation process. By making a few adjustments and planning ahead, you can create a safe and supportive environment that facilitates healing and helps you regain mobility more quickly. Here are some important tips to help you get your home ready:
- Clear Pathways: Remove any obstacles or tripping hazards such as rugs, electrical cords, and clutter from walkways. Ensure there is ample space for using a walker or crutches.
- Set Up a Recovery Area: Arrange a comfortable area on the main floor where you will spend most of your time. Include essential items like a recliner or chair with a firm cushion, a small table for necessities, and a phone or tablet for communication.
- Install Safety Aids: Add grab bars in the bathroom, especially near the toilet and shower. Consider installing a shower chair and a hand-held showerhead to make bathing safer and more comfortable.
- Lighting: Ensure all areas are well-lit to avoid any accidents. Night lights in hallways and bathrooms can be particularly helpful.
- Cook and Freeze Meals: Prepare and freeze several meals ahead of time. This will reduce the need for cooking and ensure you have nutritious food readily available.
- Stock Up on Essentials: Make sure your pantry is stocked with easy-to-prepare foods and snacks. Consider foods that are high in protein and vitamins to aid in your recovery.
- Keep Hydration Handy: Have water bottles or a water pitcher within easy reach to stay hydrated without having to move around too much.
- Arrange for Help: Enlist a family member, friend, or professional caregiver to assist you during the initial days or weeks post-surgery. They can help with daily activities, transportation to follow-up appointments, and other needs.
- Emergency Contacts: Keep a list of emergency contacts and important phone numbers in a visible location. Make sure your support person is familiar with your medical needs and recovery plan.
- Pet Care: If you have pets, arrange for someone to help with their care, including feeding, walking, and cleaning.

Mr Freedman's Enhanced Recovery Program
Additionally, if you are a smoker, it’s crucial to cease smoking prior to your surgery. Smoking can significantly increase the risk of surgical complications, including infection and delayed wound healing. Staying active is also beneficial; we encourage continuing low-impact exercise up to the time of your surgery to promote better recovery outcomes.
Frequently asked questions
The best type of hip replacement for you depends on factors like your age, activity level, overall health, and specific hip condition, typically determined in consultation with your orthopeadic surgeon.
Yes, you will need to bring a summary of your medical history to your appointment, including any specific conditions such as bleeding disorders, blood clots, heart or lung issues, diabetes, or previous joint infections. Additionally, you may undergo further evaluations as needed.
The type of anaesthesia used for your surgery will depend on various factors, including the specifics of your condition and the surgical procedure. It may be general anaesthesia, regional anaesthesia, or local anaesthesia.
The decision between general, regional, or local anaesthesia will be made based on your medical history, the complexity of the surgery, and discussions with your anaesthesiologist and Mr Freedman.
Yes, factors such as a complex medical history, previous surgeries, anatomical variations, or unexpected findings during the procedure might extend the duration of the surgery. Mr Freedman will discuss any potential concerns with you prior to the operation.
Our locations
- Main Practice Consulting Rooms
- Other Clinic Consultations
- Surgery Operating locations
- Telehealth Consultations
Our main practice consulting rooms are located at:
Mr Ilan Freedman
Suite 2, Monash House Private Hospital
271 Clayton Road, Clayton VIC 3168.
Driving: Monash House Private Hospital is situated on Clayton Rd, across the road from Monash Medical Clinic. Clayton Road is easily accessible form Princes Highway (Dandenong Rd, North Rd or Centre Rd).
Parking: Parking available onsite (paid – inexpensive) and neighbouring streets (free)
Public transport: 3 minutes walk from Clayton Railway Station. Bus stop directly outside.
Location in the hospital: We are located on the ground floor, opposite the hospital coffee shop and next door to Capital Radiology
Mr Freedman also consults regularly at the following clinics.
Mulgrave Private Hospital Consulting Suites
Address: Blanton Dr, Mulgrave VIC 3170
Parking: Inexpensive onsite parking
The Bays Private Hospital Consulting Suites – Mornington
Address: Vale St, Mornington, 3931
Parking: Free Parking Available on site
Location: We are located in Suite 15 at The Bays.
Warragul
Address: 33 Victoria Street, Warragul 3820
Parking: Free Street Parking
Maryvale Private Hospital
Address: 286 Maryvale Rd, Morwell, 3840
Parking: Free Street Parking
Bay Street Specialist Centre
Address: Suite 4, 214 Bay Street, Brighton VIC 3186
Parking: Free Street Parking
Mr Freedman’s surgery operating locations are:
Mulgrave Private Hospital
Address: Cnr Police Rd & Gladstone Rd, Mulgrave, 3170
The Bays Private Hospital, Mornington
Address: 262 Main St, Mornington VIC 3931
Monash House Private Hospital
Address: 271 Clayton Rd, Clayton VIC 3168
Maryvale Private Hospital
Address: 286 Maryvale Rd, Morwell VIC 3840
Telehealth Consultation
We are pleased to offer telehealth appointments, allowing you to consult with Mr Freedman from the comfort of your home. Whether for a follow-up, pre-surgical consultation, or orthopaedic advice, our telehealth services provide expert care without the need to travel. Using secure and easy-to-use technology, our telehealth appointments fit seamlessly into your schedule, ensuring the same high standard of care as an in-person visit.

Get back to life sooner
We understand that seeking care for your hip or knee condition is an important decision, and we are here to provide you with the support and expertise you need.
Please take a moment to fill out the following information so that we can better understand your needs and how we can assist you.
